sciatica
and Carola Felchner, science journalistMareike Müller is a freelance writer in the medical department and assistant doctor for neurosurgery in Düsseldorf. She studied human medicine in Magdeburg and gained a lot of practical medical experience during her stays abroad on four different continents.
More about the expertsCarola Felchner is a freelance writer in the medical department and a certified training and nutrition advisor. She worked for various specialist magazines and online portals before becoming a freelance journalist in 2015. Before starting her internship, she studied translation and interpreting in Kempten and Munich.
More about the experts All content is checked by medical journalists.If it pulls painfully from the back to the leg, the sciatica is usually to blame. This slang term summarizes various complaints that originate from the sciatic nerve. Medically correct, the phenomenon is called sciatica. The cause can be, for example, a herniated disc or an inflammation. Read more about the causes, symptoms and treatment of sciatica here and find out why the sciatica does not like sitting for long periods of time and how you can prevent symptoms.
ICD codes for this disease: ICD codes are internationally recognized codes for medical diagnoses. They can be found, for example, in doctor's letters or on certificates of incapacity for work. M54M51

Brief overview
- What is sciatica? Damage to the sciatic nerve with pain that usually radiates into the leg. Doctors speak of sciatica.
- Symptoms: tingling, electric shock-like or pulling pain, numbness, signs of paralysis
- Treatment: depending on the cause and severity. Therapy options include medication, operations, physiotherapy, heat treatments, massages, etc.
- Causes: herniated disc, vertebral body injuries, joint rheumatism, inflammation, abscesses, bruises, tumors, infections, etc.
- Prognosis: With timely, correct treatment, the chances are good that the symptoms will heal completely.
Sciatica: symptoms
The sciatic nerve (sciatic nerve) is the thickest nerve in the human body. It extends over the back of the thigh and branches at knee level into its two lower leg branches, the peroneal nerve (Nervus peroneus) and the tibial nerve (Nervus tibialis). It supplies the muscles in the leg and uses its sensory components to transmit sensory reports from the lower extremities to the central nervous system.
Sciatica can cause discomfort gradually or suddenly. Doctors refer to typical sciatica pain as neuropathic pain. Many patients express themselves more clearly: Sciatica symptoms should feel like “an electric shock” or “ants tingling in the leg”. In addition, numbness and symptoms of paralysis can occur.
It is also very characteristic that the pain radiates. One then speaks of radicular pain (originating from the nerve root). This is what distinguishes sciatica from lumbago, for example. This can also occur through unhappy turning or lifting and manifests itself in sudden back pain. But this does not pull in the leg.
If the fibers of the fifth nerve root of the lumbar spine (L5) are particularly affected, the pain runs from the buttocks over the rear outer thigh via the outer knee to the anterior outer lower leg. It can even pull down to the ankle. If the first nerve root of the sacrum (S1) is damaged, the sciatica pain extends from the sacrum over the buttocks to the back of the thigh. The pain continues down the hollow of the knee and into the foot.
Radiating sciatica
If the sciatica is pinched due to a herniated disc, the pain is often exacerbated by coughing, sneezing or straining (when defecating) and movement. Urination and defecation are more rarely disturbed. If inflammation is the cause of sciatica, the pain often increases at night.
Sciatica Treatment: What To Do If You Are In Pain?
The best way to treat sciatica pain depends on the cause, severity, and duration of the discomfort. The first priority of sciatica treatment, however, is to get relief as quickly as possible, especially if it has just occurred. This is to prevent the pain from becoming chronic and a so-called pain memory from developing. Doctors understand this to mean that the central nervous system uses “learning effects” to later report pain even when there is no longer any cause.
Sometimes the body manages to heal itself or the affected nerve on its own. Often the pain subsides after a few days up to six weeks.
Tip: In the case of acute complaints, it can be helpful to put your legs up. You can build a so-called step bed yourself by lying on your back and pushing a pillow or mattress piece under your legs so that the lower legs are elevated and both the hip and knee joints are bent at a right angle (90 degrees).
If the pain does not improve or is very severe from the start, the sciatica can be treated in three ways: with medication, other conservative therapies (physiotherapy, etc.) and surgery.
Drug treatment of sciatica
Sciatica pain can be relieved with pain relievers. In doing so, the attending physician is usually guided by the pain therapy level scheme of the World Health Organization (WHO). This scheme consists of the three stages:
- Non-opioid pain relievers such as acetaminophen, ibuprofen, or diclofenac
- weak opioid pain relievers (such as tramadol) in combination with non-opioids
- strong opioid pain relievers (e.g. morphine, buprenorphine or fentanyl) in combination with non-opioids.
First, attempts are made to relieve sciatica pain with non-opioid pain relievers. If these do not work well enough, the doctor can also prescribe weak opioids. Strong opioids are only used for severe pain that is difficult to treat.
Opioids are very effective pain relievers. But they can have life-threatening side effects and make you dependent. Therefore, they should only be used with caution and under medical supervision.
Sometimes the cause of sciatica can also be specifically treated with medication. Then one speaks of a specific sciatica therapy:
For example, if an infection triggers the pain, the doctor can prescribe antibiotics (against bacteria) or antivirals (against viruses). Antibiotics may also be needed if there are complications, such as a collection of pus pressing on the sciatic nerve.
-
"Always have a doctor clarify sciatica"
Three questions for
Dr. med. Joachim Mallwitz,
Specialist in Orthopaedics -
1
How do I know if my sciatica is causing problems?
Dr. med. Joachim Mallwitz
Sciatica is a pain in the leg that originates from the sciatic nerve. The pain begins in the buttocks and runs down to the foot - these are the regions that the nerve supplies. In doing so, it migrates on the back of the thigh and the back and side surfaces of the lower leg up to the toes. Sometimes a sensory disorder or muscle weakness also occurs. Sciatica can affect anyone because there are so many different causes.
-
2
Are there any quick reliefs to relieve the pain?
Dr. med. Joachim Mallwitz
Basically, let the doctor clarify the pain first! What you can then do yourself depends on the cause. If there is an inflammation behind it, appropriate medication can help. Sometimes the nerves are also constricted, for example because an intervertebral disc is pressing on them. A physiotherapist can then show you relief positions for the nerve, which you can later adopt independently. Warmth and pain medication can also provide relief.
-
3
As an expert, do you have any special advice for those affected?
Dr. med. Joachim Mallwitz
Depending on what caused the sciatica, you can prevent recurrence. In the event of a malfunction of the musculoskeletal system, for example, the patient is given an exercise program to take at home. Among other things, he learns to improve his movement coordination.
-
Dr. med. Joachim Mallwitz,
Specialist in OrthopaedicsDr. med. Joachim Mallwitz is the founder of the Am Michel Back Center in Hamburg, which has been dealing with the treatment of musculoskeletal disorders on an interdisciplinary basis since 2001.
More conservative sciatica treatment
In addition to medication, there are other conservative (non-surgical) therapy options for sciatica. Physiotherapy can relieve sciatica pain and improve the prognosis in the long term. Depending on the method, it can loosen tense muscles, stabilize and strengthen the spine and correct any incorrect or relieving postures. For example, exercise therapy (physiotherapy, back training), heat treatments or massages are used. The therapist will choose appropriate treatments for each patient.
This helps with acute pain
Another important approach in so-called multimodal treatment is behavioral therapy. It should help the patient to cope better with the symptoms. In addition, the aim is to prevent the patient from taking too much care and exercising less for fear of the sciatic pain. That jeopardizes the long-term success of the treatment. The behavioral approach therefore plays an important role in modern sciatica treatment.
Bed rest may be advisable in acute pain. In order to prevent future sciatica complaints, those affected should exercise a lot. When working at a desk, for example, it is advisable to get up from time to time and do light gymnastics (back exercises, etc.). This relieves and strengthens the back and the intervertebral discs.
Surgical sciatica treatment
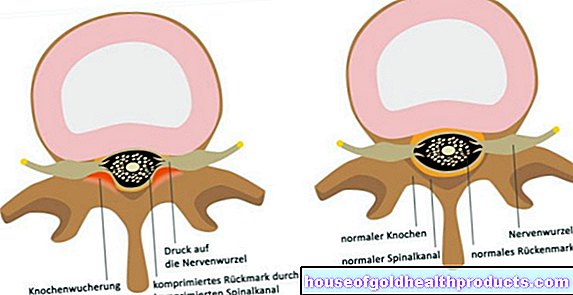
Surgery is rarely necessary for sciatica. This can be the case, for example, if a herniated disc causes serious symptoms (such as defecation disorders, symptoms of paralysis or severe pain that is difficult to treat). Sometimes sciatica is also the result of a narrowing of the spinal canal in the lumbar region (lumbar spinal stenosis). Then, under certain circumstances, an operation can also be useful.
Today, such operations are usually carried out in a minimally invasive manner. The surgeon does not make a large incision in order to have a direct view of the area to be operated on. Instead, he makes several small incisions through which he introduces fine optical and surgical instruments into the body.
Sciatica: examinations and diagnosis
Sciatica can be very painful, but it usually goes away on its own within days to weeks. However, if you have persistent or recurring symptoms, you should see a doctor.
In general: If back pain is accompanied by numbness or paralysis in the leg and / or disorders of bowel and bladder emptying, you should urgently consult a doctor!
The doctor will first ask you in detail about your medical history (anamnesis). He may ask the following questions:
- Since when do you have the pain?
- Did the symptoms arise suddenly and in connection with certain stresses?
- How would you describe the pain (e.g. as shooting or electrifying)?
- Where exactly is the pain? Do you radiate?
- What will give you relief?
- What is your profession?
- Is your everyday life affected by the sciatic pain?
During the following clinical exam, your doctor will first look at your back and legs. He pays attention to possible misalignments and checks the mobility of the joints, the strength of the muscles and your reflexes. It also tests the sensitivity to touch and the feeling on the legs by stroking the skin and letting you identify the place where it touched you.
Your doctor uses the so-called Lasègue test to check whether the nerve roots of the lower spinal cord are irritated. You lie on your back and the doctor lifts your stretched leg. If the sciatic nerve is pinched or otherwise irritated, pain in the back occurs halfway up, which shoots into the leg.
To find the cause of the symptoms, the doctor can carry out further examinations, for example magnetic resonance imaging (MRI or magnetic resonance imaging) or computed tomography (CT). Such imaging procedures are especially important when there is paralysis or discomfort.
To determine the location and extent of the nerve damage, the doctor can use electrodes to measure muscle activity (electromyography = EMG) and nerve conduction speed (electroneurography = ENG).
If a sciatic nerve infection is suspected, the doctor will draw blood from you to determine the inflammation levels and identify any pathogens (such as Borrelia). Cerebral fluid (liquor) may also need to be taken and analyzed. To do this, the doctor sticks a needle through the skin of the lower back and carefully pushes it into the spinal canal next to the spinal cord in order to take a small CSF sample (CSF puncture).
Lumboischialgia
Lumboischialgia manifests itself in a similar way to "classic sciatica" (sciatica): Those affected report, for example, pulling pains, tingling sensations and numbness in the leg. Muscle weakness is also possible.
In contrast to sciatica, not only is the sciatic nerve irritated in lumbar disease, but also the nerves that leave the spinal cord at the level of the lumbar spine. Accordingly, the pain comes less from the buttocks than from the lower back.
You can find out more about symptoms, diagnosis and treatment in the article Lumboischialgia!
Sciatica: causes and risk factors
The main cause of sciatica problems is a herniated disc or its precursor, the protruding disc. But there can also be other diseases behind it if they press on nerve roots and fibers of the sciatica. These include, for example:
- Vertebral body injuries
- Tumors
- Rheumatoid arthritis
- Inflammation of the intervertebral disc and the surrounding vertebral bodies (spondylodiscitis)
- Collections of pus (abscesses)
- Bruising (hematoma)
Another cause of sciatica irritation can be an infection, such as Lyme disease. The bacterial pathogens causing this infection (Borrelia) are transmitted by ticks. Herpes viruses in shingles (herpes zoster) can also cause sciatica problems.
Sciatica in Pregnancy
Back pain is not uncommon during pregnancy. However, the sciatic nerve is rarely behind it. Instead, the pain is mostly due to pregnancy-related factors such as the growing weight in the abdomen and the hormonal loosening of the ligament structures.
However, this does not mean that sciatica (similar) symptoms during pregnancy should be taken lightly. Since, for example, a herniated disc or other serious causes are also possible, affected women should definitely see a doctor.
If the doctor actually diagnoses sciatica, it is usually treated with physiotherapy. Painkillers are not used or only to a limited extent during pregnancy for the benefit of the unborn child.
You can read everything you need to know about sciatica in expectant mothers in the article Sciatica in pregnancy.
Sciatica: disease course and prognosis
The trigger is decisive for the course of the complaint in sciatica. If therapy is started early, the prognosis for sciatic nerve pain is good. If surgery is not necessary, good pain therapy in conjunction with physiotherapy started in good time can usually shorten the course of the disease considerably.
It is important to specifically strengthen the back and abdominal muscles with regular exercises and sport. A strong muscle corset relieves and stabilizes the spine. This can alleviate or prevent back problems.
Patients should also learn how to behave in a way that is easy on their backs (for example when working at a desk or lifting heavy loads). This can relieve existing symptoms and prevent new sciatica problems.
In addition, social and psychological factors also influence the course and prognosis of back pain, including sciatica. For example, loneliness, depressive mood and stress can cause or worsen the symptoms. They can also help make back pain chronic and make pain relievers less effective. That means:
An intact social life, the support of relatives and friends, good conditions in the workplace, a trusting relationship with the treating doctor and a positive mood can significantly improve the prognosis of sciatica pain.
Additional information:
Guideline:
- Guideline "Disc-related sciatica" of the German Society for Orthopedics and Orthopedic Surgery and the Professional Association of Orthopedic Doctors